Candida auris & ESKAPE Bacteria Pathogen Testing
Surface Testing for Disease Prevention and Outbreak Investigations
Environmental Surfaces in Disease Transmission
It has been well-established that environmental surfaces play an important role in the endemic and epidemic transmission of certain pathogens that cause healthcare-associated infections1. These bacteria (especially the so-called ESKAPE bacteria; see below) and certain fungal/yeast pathogens (especially Candida auris2) share the ability to be shed from infected or colonized patients, survive as infectious agents on dry surfaces for extended periods, are difficult to treat because of multiple drug-resistances (MDRs), and are difficult to eradicate from their environmental locations, even with the recommended cleaning and disinfection agents and practices.
Microbial Surveillance of Touch Surfaces
Because of the complexity in the different types of touch surfaces in healthcare institutions, it is difficult to confirm the complete absence of any one pathogen on those surfaces, despite the rigor of the cleaning and disinfection program in place. As a result, the requirements for surface hygiene in clinical spaces are not as well characterized as are the microbial safety requirements and standards for hospital water or air.
Nevertheless, as shown in a recent study by Watkin and colleagues from the University College London3, a routine surface hygiene microbial surveillance program of touch surfaces in a hospital can not only help to identify the source of infectious diseases outbreaks when they occur (Rapid Response), but may also help to prevent outbreaks of these infectious diseases in the first place (Disease Prevention)
1Otter, J.A. et. al. (2013). Evidence that contaminated surfaces contribute to the transmission of hospital pathogens and an overview of strategies to address contaminated surfaces. Am. J. Infect. Control. 41: S6-S11.
2Du, H., et al. (2020). Candida auris: Epidemiology, biology, antifungal resistance, and virulence. PLoS Pathog. 16 (10): e1008921.
https://journals.plos.org/plospathogens/article?id=10.1371/journal.ppat.1008921
3Watkin et al., How can monitoring touch surfaces for microbial contaminants support infection control practice?; Presented at: ASM Microbe; June 15-19, 2023, Houston, TX.
Candida auris
A drug-resistant pathogen that spreads in healthcare facilities.
Candia auris (C. auris) is a yeast that demonstrates an ability to evade host innate immunity4 as well as to express multi-drug resistance. C. auris was first identified in 2009 in Japan (CDC.gov, n.d.; Weerasinghe et al., 2023) and has been present in the United States since 2013. C. auris is one of the leading causes of invasive candidiasis, a healthcare acquired infection (HAI) that often presents in immunocompromised individuals. Treatment of invasive candidiasis caused by C. auris is profoundly difficult. C. auris can easily be misidentified as other Candida species, and due to its multi-drug resistance, the effectiveness of most antifungals is limited. This presents a difficult scenario, where a patient infected with C. auris could be subject to delayed and ineffective treatment. All these factors may contribute to the high mortality rate of 30-60% that has been observed so far.
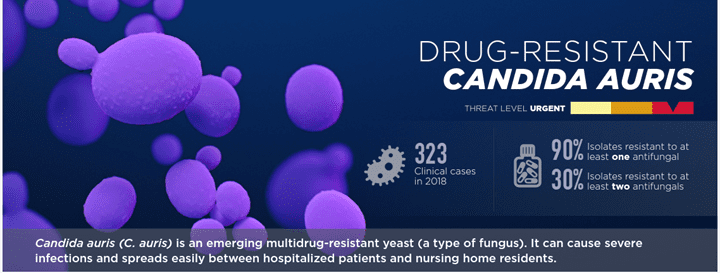
CDC Fact Sheet Link: https://www.cdc.gov/fungal/candida-auris/fact-sheets/index.html
4Weerasinghe, H., Simm, C., Djajawi, T., Tedja, I., Lo, T. L., Shasha, D., Mizrahi, N., Olivier, F. A., Speir, M., Lawlor, K. E., Ben-Ami, R., & Traven, A. (2023). Candida auris evades innate immunity by using metabolic strategies to escape and kill macrophages while avoiding antimicrobial inflammation. Biorxiv. https://doi.org/10.1101/2023.02.28.529319
Other Infectious Agents of Concern:
ESKAPE+C
ESKAPE is a well-recognized clinical acronym comprising the scientific names of six (6) bacterial pathogens, including their vancomycin-resistant (VR), methicillin-resistant (MR), and carbapenem-resistant (CR) variants. the acronym is an accurate reference to the ability of these pathogens to “escape” the killing effects of commonly used antibiotics.
Enterococcus faecium + VRE
Staphylococcus aureus + MRSA
Klebsiella pneumoniae + CRE
Acinetobacter baumannii + CR
Pseudomonas aeruginosa + CR
Enterobacter species + CRE
Another bacterium is often added to this group is the spore-forming bacterium Clostridioides difficile, leading to a new acronym called ESKAPE + C. These seven bacteria are the major causes of life-threatening hospital-acquired infections in immunocompromised and critically ill patients who are most at risk of infection via transmission from other colonized patients or staff, contaminated hospital surfaces or equipment, or hospital water. They are additionally problematic because of the increasing antibiotic resistance found in many of the clinical isolates. Infections associated with ESKAPE pathogens have become a major obstacle in choosing an effective therapeutic strategies5.
5Mulani, M.S., et al. (2019). Emerging strategies to combat ESKAPE pathogens in the era of antimicrobial resistance: A review. Frontiers Microbiol. Immunol. 10: 1-24.
https://www.frontiersin.org/articles/10.3389/fmicb.2019.00539/pdf
Candida auris and ESKAPE+C Testing
Analyses can be ordered individually, by select grouping, or all at the same time.
All analyses for a sample site can be run from a single EST supplied surface swab.
-
-
-
Candida auris
-
Enterococcus faecium + VRE
-
Staphylococcus aureus + MRSA
-
Klebsiella pneumoniae + CRE
-
Acinetobacter baumannii + CR
-
Pseudomonas aeruginosa + CR
-
Enterobacter species + CRE
-
Clostridioides difficile (C. diff)
-
Others pathogens of interest in your institution upon request
-
-
Don’t let Candida auris, ESKAPE+C, or other drug-resistant pathogens become the source of an outbreak or death at your facility.
EST can help you with:
Candida auris and ESKAPE+C Disease Prevention and Outbreak Response
- Investigation of Potential Reservoirs of Pathogens
- Collection of Environmental Samples
- Laboratory Analyses of Surface Samples
- Infection Prevention Consultation
- Interpretations and Recommendations


